Statistics on Physician Burnout Explained
Explore the latest statistics on physician burnout. Understand the data behind the crisis and learn how to build a more sustainable career in medicine.

The numbers on physician burnout tell a story of a system pushed to its absolute limit. It’s a crisis that’s been simmering for years, but the recent pandemic threw gasoline on the fire, exposing just how fragile things really are.
Today, nearly half of all U.S. physicians are dealing with burnout. Let’s dig into the data to see how we got here.
Unpacking the Physician Burnout Epidemic
To really get a handle on the scale of this problem, you have to look at the hard numbers. Think of the healthcare system as an electrical grid that’s been running at 110% capacity for decades. The pandemic was like a massive, unprecedented power surge that nearly blew the circuits for good.
The data from the last few years looks like a rollercoaster. A landmark national survey from the American Medical Association found that a staggering 62.8% of physicians reported at least one burnout symptom in 2021. That’s a huge jump from 38.2% in 2020 and way above anything we saw pre-pandemic.
By 2023, the rate cooled off to 45.2%. While that’s an improvement, it’s still a deeply troubling number—and far higher than what you’d find in almost any other profession.
Physician Burnout Rates At A Glance
Here’s a quick summary of the key burnout statistics from the last few years. It paints a clear picture of the volatility and the persistent nature of this crisis.
| Year/Report | Reported Burnout Rate | Key Context |
|---|---|---|
| 2020 (AMA) | 38.2% | Pre-pandemic baseline, already indicating significant professional stress. |
| 2021 (AMA) | 62.8% | The peak of the pandemic surge, representing a high-water mark for burnout. |
| 2023 (Medscape) | 45.2% | A post-peak decline, but still nearly half of the physician workforce. |
This table isn't just a list of numbers; it’s a timeline of a profession in distress. The peak in 2021 was a breaking point, and the slow recovery since then shows the underlying problems were never solved.
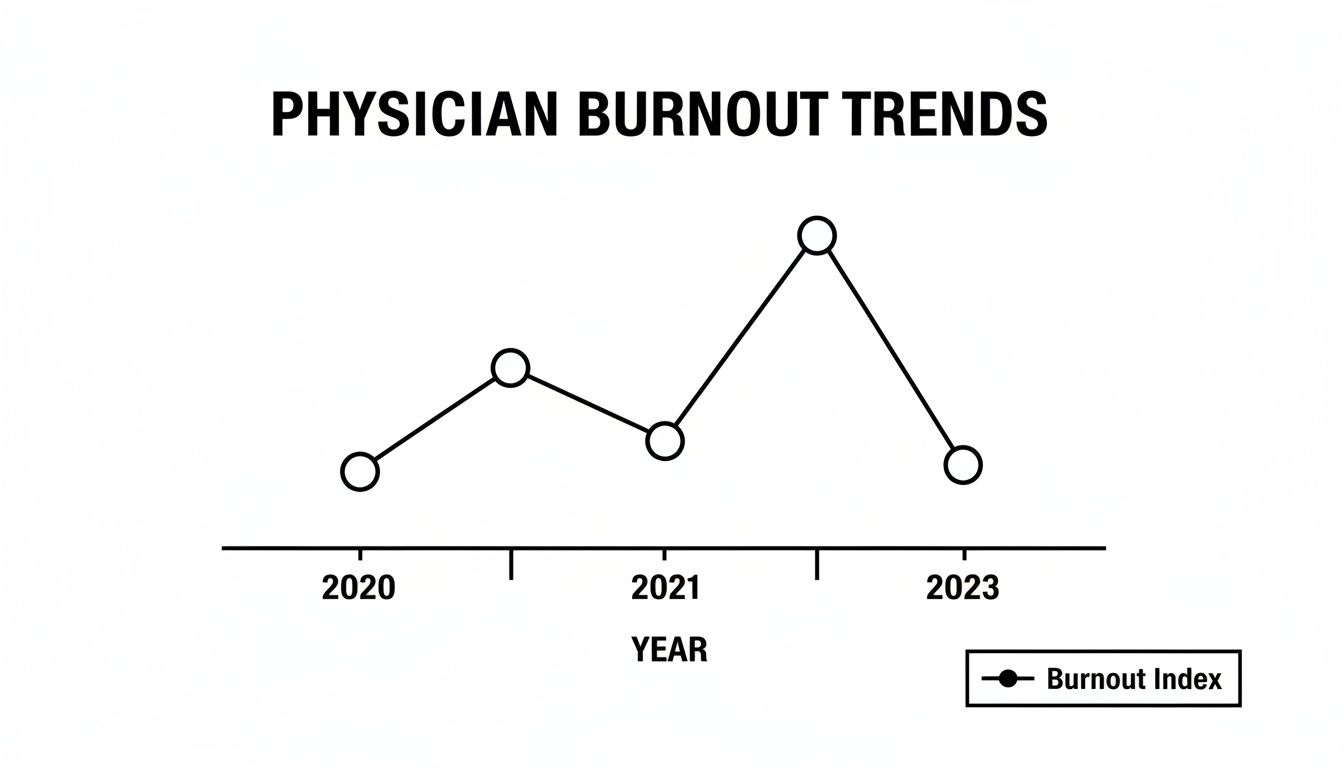
This chart drives the point home. You can see the massive spike in 2021 followed by a gradual, but incomplete, return toward the baseline. It proves that while the acute crisis of the pandemic has passed, the chronic illness of burnout remains.
The Core Components of Burnout
Burnout isn’t just about being tired after a long week. It’s a specific syndrome with three distinct parts. If we want to fix this, we first have to understand what we’re looking at.
- Emotional Exhaustion: This is that bone-deep feeling of having nothing left to give. It’s when you’re so emotionally and physically drained that you can’t muster the energy for your patients, your family, or yourself.
- Depersonalization (or Cynicism): This is the emotional armor you put on to survive. It looks like a cynical, detached attitude toward your work and your patients. You start seeing people as diagnoses or tasks instead of human beings.
- Reduced Sense of Personal Accomplishment: This is the feeling that your work doesn't matter anymore. You feel incompetent, ineffective, and question whether you’re actually making a difference, despite all the years of training and hard work.
Burnout is not a sign of individual failure. It's a symptom of a dysfunctional work environment. The numbers make it clear: this is a systemic problem, not a collection of personal struggles.
Recognizing these signs in yourself is the first step. If you're wondering where you fall on the spectrum, our proprietary Burnout Index can give you some personalized insight.
Now that we're grounded in the data, we can start to unpack what’s causing these trends and, more importantly, what we can actually do about it.
Mapping Burnout Across Specialties and Demographics
 Physician burnout isn't a one-size-fits-all problem. It hits different clinicians with wildly different levels of intensity. To really get a handle on the statistics, you have to look at a more detailed map—think of it like a weather map where some regions are stuck in a perpetual storm while others see only passing clouds.
Physician burnout isn't a one-size-fits-all problem. It hits different clinicians with wildly different levels of intensity. To really get a handle on the statistics, you have to look at a more detailed map—think of it like a weather map where some regions are stuck in a perpetual storm while others see only passing clouds.
This detailed view shows us exactly which specialties, demographic groups, and career stages are most vulnerable. By breaking the data down, we can get past broad statements and pinpoint the real pressure points in the system. Getting this granular is the only way for clinicians to find sustainable careers and for employers to build healthier workplaces.
The numbers are clear: frontline specialties carry the heaviest load. These are the fields where the storm of high stress, brutal hours, and intense patient acuity almost never lets up.
The Frontline Fields Feeling the Heat
Emergency medicine consistently tops the charts for burnout rates. It’s a perfect storm of a chaotic, high-stakes environment, the grind of shift work, and intense emotional demands that lead directly to exhaustion and cynicism.
Primary care isn't far behind. Fields like internal and family medicine show alarmingly high numbers year after year. These doctors are often buried under massive patient panels, endless administrative work, and the weight of being the healthcare system’s gatekeepers. The strain is immense, and the statistics prove it.
For instance, a striking 63% of emergency physicians reported burnout in 2024. And it's a similar story for primary care—a 2022 survey across 10 countries found U.S. primary care doctors had a 45% burnout rate, the highest of the group. You can dig into more national physician burnout data to see the full scope of these disparities.
The bottom line is that your medical specialty has a direct, measurable impact on your risk of burnout. The inherent work environment, patient acuity, and administrative burden are powerful predictors of whether you’ll thrive or just survive.
This is a critical insight for any physician planning their career or thinking about making a change. The specialty you choose, or even the specific environment you work in, can dramatically shape your long-term satisfaction in medicine.
Demographic Disparities in Burnout Rates
Beyond specialty, demographic factors play a huge role. The data shows clear patterns based on gender and career stage, exposing systemic issues that go far beyond the day-to-day grind of clinical practice.
One of the most consistent findings is the gender gap. Study after study confirms that women physicians report higher burnout rates than their male colleagues, even within the same specialty. This points to the extra stressors female clinicians often face, from navigating workplace bias to shouldering a disproportionate amount of household and caregiving duties.
The data consistently highlights a few particularly vulnerable groups:
- Women Physicians: Consistently report higher rates of emotional exhaustion and overall burnout, with some studies showing rates 10-20% higher than their male counterparts.
- Early-Career Physicians: Residents and new attendings in their first five years face a brutal combination of pressure, long hours, and a steep learning curve that fuels high burnout.
- Mid-Career Physicians: This group is often caught in the "sandwich generation," trying to balance a demanding clinical career with caring for both young children and aging parents.
These statistics on physician burnout paint a clear picture: this crisis isn't uniform. It has epicenters in certain specialties and disproportionately hammers specific demographic groups. By mapping these high-risk areas, both individual doctors and healthcare institutions can start building smarter, more targeted defenses against this professional hazard.
Uncovering the Root Causes of Clinician Burnout
To really get why physician burnout is so rampant, we have to look past the symptoms and dig into the systemic roots of the problem. This isn't about a lack of personal resilience. It’s a completely natural response to a work environment choked with friction, inefficiency, and impossible demands.
Think of a physician’s daily energy as a finite resource, like a bucket of water. Every bureaucratic task, every extra hour spent on charting, every moment fighting with technology—each one pokes a small hole in that bucket. Over time, those little leaks become a torrent, draining a clinician's ability to provide compassionate, effective care.
The data consistently points back to the same set of systemic issues creating these leaks. By pinpointing these core drivers, we can stop seeing the crisis as an unavoidable part of medicine and start treating it as a problem with identifiable, solvable causes.
The Crushing Weight of Administrative Work
The single biggest drain on a doctor's well-being isn't the complexity of patient care. It's the mountain of administrative work that comes with it. Electronic health records (EHRs) were supposed to streamline workflows, but they’ve often done the exact opposite, turning highly trained physicians into data-entry clerks.
This phenomenon of "pajama time"—spending hours charting late at night after a full clinical day—is a primary driver of emotional exhaustion. It's a fundamental betrayal of a physician's training. You spend years learning to diagnose and heal, only to find a huge chunk of your day is consumed by clicking boxes and wrestling with clunky software.
This administrative burden is the number one culprit. According to a 2024 Medscape report, a staggering 58% of physicians cited bureaucratic tasks like charting and paperwork as the main reason for their burnout. This was followed closely by long working hours (38%) and a lack of respect from administrators or colleagues (37%). You can find more details about how EHR documentation fuels physician burnout on fiercehealthcare.com.
Unsustainable Workloads and Long Hours
Beyond the paperwork, the sheer volume and intensity of clinical work are major forces in the burnout crisis. The healthcare system often runs on a volume-based model, pushing clinicians to see more patients in less time. This relentless pace leaves little room for thoughtful reflection, deep patient connection, or even basic needs like a lunch break.
The constant time pressure is made worse by ridiculously long workweeks. The same 2024 report found that 40% of physicians work 51-60 hours per week, and another 17% work over 60 hours. When you combine those demanding schedules with the emotional weight of caring for the sick, the path to exhaustion gets alarmingly short.
The expectation of perpetual availability—through on-call duties, weekend rounds, and overflowing inboxes—erodes the critical boundary between professional and personal life, making true recovery nearly impossible.
This relentless demand is a key reason why jobs with built-in boundaries—like those explicitly marked "No Call" or "No Weekends"—are becoming a lifeline for clinicians seeking a sustainable career.
Loss of Autonomy and Professional Respect
A third powerful driver of burnout is the slow erosion of professional autonomy. Many physicians today feel like cogs in a massive machine, their clinical judgment hemmed in by insurance mandates, hospital protocols, and administrative oversight. This lack of control over their own practice environment breeds a profound sense of powerlessness and frustration.
This feeling is often amplified by a perceived lack of respect from the very systems they work in. When clinicians feel their expertise is undervalued and their concerns about patient safety or workload are dismissed, it feeds a deep-seated cynicism and depersonalization. These aren't just morale issues; they are direct drivers of the burnout statistics we see across the board.
Fixing these root causes requires a fundamental shift in how healthcare organizations structure work and value their clinical staff. It's about more than wellness apps and yoga sessions; it's about redesigning the job of being a doctor to be sustainable, respectful, and focused on what actually matters: the patient.
The True Cost of Physician Burnout
Physician burnout is more than just a bad day or a tough week. It's a full-blown systemic crisis, and it comes with a steep price tag that ripples across the entire healthcare landscape.
This isn't just a wellness issue felt in hospital hallways or on-call rooms. The effects show up in patient outcomes, on financial balance sheets, and in the lives of clinicians. When a doctor is running on empty, the consequences are tangible, measurable, and deeply concerning for everyone involved.
Patient Safety Is on the Line
One of the most frightening consequences of physician burnout is its direct link to medical errors. An exhausted, emotionally depleted doctor is simply not equipped to perform at the intensely high level modern medicine demands.
It’s not a small statistical blip. A major meta-analysis confirmed that physicians experiencing burnout have more than double the risk of being involved in a patient safety incident. Think about that for a second. That's like doubling the odds of a system failure every time a burned-out clinician prescribes a medication, reads a lab result, or performs a procedure.
"The epidemic of physician burnout could be responsible for more medical errors than even unsafe healthcare settings, which accounts for 100,000 to 200,000 deaths per year."
This puts the crisis in stark perspective. Burnout isn't a secondary wellness concern; it's a primary patient safety problem. It also creates a vicious cycle: making an error can crank up feelings of guilt and incompetence, pouring more fuel on the burnout fire and raising the risk of future mistakes.
The Staggering Financial Drain of Turnover
For healthcare organizations, ignoring burnout is an incredibly expensive mistake. The cost of physician turnover is enormous, turning a workforce problem into a major budget crisis.
Replacing a single physician isn't a simple matter of posting a job opening. The real cost to replace just one doctor often lands somewhere between $500,000 and over $1 million. This number covers everything from:
- Recruitment: Search firm fees, advertising, and the whole interview process.
- Hiring and Onboarding: Credentialing, administrative costs, and training for the new doctor.
- Lost Revenue: This is the big one. Significant income vanishes during the months a position stays empty and while the new physician slowly ramps up to a full patient load.
It's happening everywhere. A 2024 poll found that 27% of medical groups lost at least one physician in the last year specifically because of burnout. When a quarter of all organizations are bleeding talent like this, the replacement costs skyrocket into the millions, pulling money away from patient care and much-needed system improvements.
All told, a comprehensive analysis estimated that burnout-related physician turnover and reduced clinical hours cost the U.S. healthcare system around $4.6 billion a year. You can dig into the full burnout's economic impact for yourself.
The Personal Toll and Workforce Exodus
Beyond the numbers, burnout exacts a heavy personal price on physicians, pushing many to question their entire career path. The high rates of depression, anxiety, and even suicidal thoughts among clinicians are well-documented—it's the human cost of a punishing, often unsupportive system.
This personal crisis is fueling a mass exodus from the workforce. We're seeing scores of experienced physicians choosing to cut back their hours, pivot to non-clinical roles, or simply take early retirement to get away from the relentless pressure. This brain drain weakens our entire healthcare infrastructure. It means longer wait times for patients, heavier workloads for the clinicians who stay, and a devastating loss of mentorship for the next generation of doctors.
How to Build a Burnout-Resistant Medical Career
 Scrolling through the burnout statistics can feel defeating. But it doesn't have to be. Think of this data not as a depressing headline, but as your roadmap—the intelligence you need to stop reacting to a broken system and start designing a career that can actually withstand it.
Scrolling through the burnout statistics can feel defeating. But it doesn't have to be. Think of this data not as a depressing headline, but as your roadmap—the intelligence you need to stop reacting to a broken system and start designing a career that can actually withstand it.
It’s like being a pilot. You wouldn't take off without checking the weather and steering clear of storm systems. The data on burnout is your weather map. It shows you exactly where the turbulence is: the high-burnout specialties, the punishing work cultures, and the soul-crushing administrative burdens.
Armed with this information, you can shift from just surviving to strategically building a professional life that works for you. It’s a powerful change in perspective that puts you back in control.
Using Data to Filter Your Job Search
The first step is turning these big-picture numbers into a practical filter for your job search. We know that administrative work is the #1 driver of burnout, cited by 58% of physicians. We also know that insane hours and a lack of respect aren’t far behind.
So, the goal becomes simple: find jobs that minimize these exact pain points from day one.
Start treating job descriptions like you would a patient chart—look for the data. Hunt for keywords that signal a healthier environment. These are your green flags, clues that an employer actually gets it and is trying to build a better system.
Your burnout-resistant filter should actively seek out:
- Roles with Firm Boundaries: Prioritize job posts that explicitly state "No Call," "No Weekends," or "No Nights." These aren't just nice perks; they are structural walls protecting your time to recover.
- Positions with Real Support: Look for mentions of scribes, strong nursing teams, or dedicated administrative staff. These are the roles that directly fight back against the bureaucratic sludge.
- Manageable Patient Volume: This one can be trickier to spot. But phrases like "quality-focused care" or "extended appointment times" often hint at a system that values thoroughness over churn.
By focusing your search this way, you stop hoping for a good fit and start methodically selecting for one. You can find curated listings of these types of roles by exploring opportunities like part-time physician jobs, which often have these protections baked right in.
Mastering the Art of the Interview
Okay, you landed an interview. Now your job is to verify everything the posting promised. This is your chance to get on-the-ground intelligence about the workplace culture. Don't let them run the whole show—come prepared with targeted questions that reveal the reality of the daily grind.
The interview is a two-way street. You aren't just a candidate being evaluated; you are a highly skilled professional assessing whether an organization is worthy of your expertise and energy.
Of course, building a sustainable career also requires protecting your own well-being. A job that respects your off-hours makes it possible to adopt practices to improve sleep quality naturally—a non-negotiable for resilience in this field.
During your interview, ask direct questions that cut to the chase:
- "What is the average daily patient census for a physician in this role?"
- "Can you walk me through the administrative and scribe support provided?"
- "How does this organization protect a clinician's personal time?"
- "What's the charting culture like? What happens if it spills into evenings or weekends?"
The answers—and just as importantly, how they answer—will tell you everything you need to know. This proactive vetting is your best defense against ending up in another job that looks great on paper but is a fast track to burnout in practice.
A Strategic Imperative for Healthcare Employers
For healthcare employers, it's time to reframe the entire conversation around physician burnout. This is no longer a "soft" HR issue or a simple line item in the wellness budget. The data is screaming at us: tackling burnout is a core business strategy, absolutely essential for organizational stability, patient safety, and your bottom line.
Ignoring the warning signs is a losing game. Organizations that refuse to create sustainable work environments will continue to bleed talent, watch costs spiral, and see their quality of care plummet. Getting proactive with systemic change isn't just the right thing to do—it's a requirement for survival in a brutally competitive healthcare market.
The Financial Case for Prioritizing Well Being
Let's talk numbers, because this is where the argument becomes undeniable. The cost to replace a single physician can run anywhere from $500,000 to over $1 million once you factor in recruitment, hiring, and the massive revenue lost while the position sits empty.
And this isn't a rare occurrence. A 2024 MGMA poll found that 27% of medical groups lost at least one physician specifically due to burnout-related turnover. Those costs multiply fast. This reality means that proactive retention—strategies that genuinely improve work-life balance and slash administrative headaches—offers a staggering return on investment. You can dig into more of the findings from the MGMA survey on burnout and turnover.
Investing in clinician well-being isn't an expense; it's an investment in your most valuable asset. The ROI is measured in lower turnover, fewer medical errors, and a more resilient, engaged workforce capable of delivering superior patient care.
Seen this way, every dollar spent redesigning a clunky workflow or hiring another scribe isn't a cost center. It's an insurance policy against the multimillion-dollar catastrophe of watching your best doctors walk out the door.
Actionable Strategies for Building a Better Workplace
Truly moving the needle on burnout takes a lot more than free yoga classes and wellness apps. It demands a real commitment to rethinking how clinical work is designed from the ground up. Employers have to attack the root causes the burnout statistics point to—the systemic drains on a physician's energy and passion.
Here are a few data-backed strategies that actually work:
- Redesign Roles to Minimize Bureaucracy: Get serious about offloading administrative junk from clinicians' plates. That could mean hiring more scribes, investing in an EHR that doesn't actively fight its users, or creating dedicated support teams to wrestle with prior authorizations.
- Offer Genuine Flexibility: Stop paying lip service to flexibility and actually provide it. This means creating viable part-time roles, offering hybrid or remote work where it makes sense, and giving physicians more direct control over their own schedules.
- Rethink Mandatory Burdens: Take a hard look at legacy requirements like mandatory call schedules, weekend shifts, and after-hours charting. For many specialties, these are primary drivers of exhaustion and can often be redesigned, shared more equitably, or even eliminated.
Building a workplace that's resistant to burnout requires a deep understanding of supportive HR practices. Bringing in specialized HR advisors for healthcare businesses can provide critical guidance on creating an environment that respects a physician's time, expertise, and humanity. In the end, this isn't just about supporting your staff—it's about building a powerful competitive advantage that attracts and keeps the very best talent.
Common Questions About Physician Burnout
All this data can bring up a lot of questions. Let's break down some of the most common ones and how you can use the answers to shape your career.
What Is the Single Biggest Statistical Driver of Physician Burnout?
It's the paperwork.
Hands down, bureaucratic tasks like charting and wrestling with the electronic health record (EHR) are the top driver. Nearly 60% of physicians point to this administrative slog as their biggest source of stress.
This number tells a critical story: if you want to avoid burnout, you need a role with smart, streamlined workflows or the support staff to handle the busywork.
Are Burnout Rates Improving Since the Pandemic?
Yes, but don't get too excited. The numbers have definitely improved since the peak of the COVID-19 crisis. According to the AMA, rates dropped from a staggering 62.8% in 2021 to a still-too-high 45.2% by 2023.
While that's a positive shift, it's crucial to see the bigger picture. The current rate is still way higher than for the average American worker. It proves that the pandemic didn't create the burnout problem—it just poured gasoline on a fire that was already burning.
Burnout is a system problem, not an individual failing. The data confirms that while acute pressures may ease, the underlying causes of chronic professional stress persist across healthcare.
How Can I Use These Burnout Statistics in My Job Search?
Use this data to get surgical with your job search. Stop just looking for any new job and start filtering for roles that actively eliminate the known causes of burnout.
This means hunting for positions that advertise things like "No Call" or "No Weekends." Look for jobs with reasonable patient loads or dedicated administrative support. This isn't being picky; it's being strategic about building a sustainable career.
If you're not sure how your current situation stacks up, run your numbers through our physician burnout calculator to get a baseline. This proactive approach lets you design a work-life that actually works.
At WeekdayDoc, we connect clinicians with burnout-friendly jobs that respect your time and expertise. Find your next role at https://www.weekdaydoc.com.