Calculating rvu: A Quick Guide to RVU-Based Pay and Negotiation
Discover calculating rvu basics, how wRVUs, modifiers, and conversion factors affect pay, and how to negotiate with confidence.

Calculating your compensation with RVUs basically means breaking down every medical service into three core parts: physician work, practice expense, and malpractice risk. This system is how Medicare and tons of private payers put a number on your clinical effort, which then gets multiplied by a dollar amount (the conversion factor) to figure out payment.
Why Understanding RVU Calculations Is Crucial for Your Career

Ever feel like your paycheck is a total black box? You’re not alone. The business of medicine runs on a complex language of codes and metrics, and at the very heart of how doctors get paid is the Relative Value Unit (RVU).
Learning to calculate RVUs isn't just some academic exercise—it's a critical skill for any modern clinician.
For most physicians, getting a handle on this system is the key to making sure your compensation is right, confidently comparing job offers, and actually having some leverage during contract talks. If you don't get this stuff, you're pretty much navigating your financial future in the dark.
The Building Blocks of Your Value
When you get down to it, every medical service is assigned a Total RVU value. This number is just the sum of three distinct components, with each one representing a different piece of the resource pie needed to provide that care.
- Work RVU (wRVU): This is all about your direct effort—the time, technical skill, mental energy, and stress involved. A standard office visit like CPT code 99213 (established patient, low complexity) has a wRVU of 1.30. Compare that to a complex surgery, and you see the difference immediately.
- Practice Expense (PE) RVU: This piece covers the overhead. Think rent, equipment, supplies, and salaries for your non-physician staff.
- Malpractice (MP) RVU: This accounts for the relative cost of professional liability insurance tied to a specific service.
By splitting a service into these three parts, the RVU system creates a standardized measuring stick for the resources consumed. It’s what ensures a routine check-up is valued differently from a high-stakes surgery, giving a more equitable foundation for reimbursement.
This knowledge is especially vital if you're exploring flexible roles. We dive deeper into how pay structures can differ in our guide on part-time physician jobs, where a solid grasp of RVUs is absolutely essential.
Ultimately, mastering these concepts gives you the power to take real control over your career and finances in an increasingly complicated healthcare world.
Breaking Down the RVU: The Three Core Components
Before we can really crunch the numbers, you have to understand that a "Total RVU" isn't some single, mysterious figure. It’s actually a composite score built from three distinct parts. Each one represents a different piece of the puzzle—the effort, the overhead, and the risk involved in any medical service.
Getting a handle on these three components is the first real step to mastering the RVU formula.
Physician Work RVU (wRVU)
This is the one you’ll hear about the most, and for good reason. The Physician Work RVU (wRVU) is meant to capture your direct effort: the time, the technical skill, the mental heavy lifting, and the stress that comes with providing a specific service.
Think of it as the core measure of your clinical productivity.
For example, a standard office visit for an established patient (CPT 99213) has a wRVU of 1.30 for 2024. That number is pretty low because the visit is relatively straightforward. On the other end of the spectrum, a major surgery could easily have a wRVU over 50. Most physician compensation models are built directly on wRVUs, linking the work you do directly to your paycheck.
Practice Expense RVU (PE RVU)
Next up is the Practice Expense RVU (PE RVU). This component accounts for the business side of medicine—all the overhead required to keep the lights on. We're talking about office rent, utilities, medical equipment, supplies, and salaries for your support staff.
Here’s a critical detail: PE RVUs are split into two categories.
- Non-Facility PE RVU: This value is higher. It's used when a service is performed in a private office where your practice is footing the entire bill for overhead.
- Facility PE RVU: This value is lower. It applies to services done in a hospital or an ambulatory surgery center, since the facility is covering most of those overhead costs.
That split explains why the exact same procedure pays more when done in your own office versus a hospital-owned clinic.
Malpractice RVU (MP RVU)
The final piece is the Malpractice RVU (MP RVU). This value accounts for the professional liability risk tied to a medical service. While it's usually the smallest of the three components, it’s still an essential part of the equation.
High-risk procedures, like complex surgeries, naturally carry a higher MP RVU. A low-risk office visit, on the other hand, will have a tiny MP RVU. This component ensures the payment model reflects the financial risk you and your practice take on.
At its core, the Total RVU is a weighted average of these three parts: your Work, the practice’s Expense, and the professional Malpractice risk. Seeing how they balance out is the key to understanding physician reimbursement.
When you look at the final calculation, the weights become clear. Physician work (wRVUs) typically makes up about 52% of the total. Practice expenses account for another 44%, and malpractice insurance risk represents the last 4%. If you want to dive deeper into the history, you can explore the Relative Value Unit system on Wikipedia.
Of course, none of this works without solid record-keeping. A deep understanding of clinical documentation improvement is non-negotiable, as it’s what justifies the codes you bill. When your documentation is on point, each RVU component is captured accurately, ensuring you get paid fairly for the work you do.
How to Calculate Total RVU Reimbursement
Once you've got a handle on the three core components—Work, Practice Expense, and Malpractice—it's time to put it all together. But calculating the final payment isn't as simple as just adding up the base RVU values. The system uses a more nuanced formula to account for regional cost differences and, crucially, to turn those abstract RVU "points" into an actual dollar amount.
The full formula for calculating a Medicare payment looks like this:
[(wRVU * Work GPCI) + (PE RVU * PE GPCI) + (MP RVU * MP GPCI)] * Conversion Factor = Payment
Let's break down the two new players in this equation: the GPCI and the Conversion Factor. These are the final pieces of the puzzle for figuring out exactly what a service is worth.
This flowchart shows how the individual RVU components, each adjusted by its specific GPCI, combine to form the Total Geographically Adjusted RVU. That total is then multiplied by the Conversion Factor to determine the final payment.
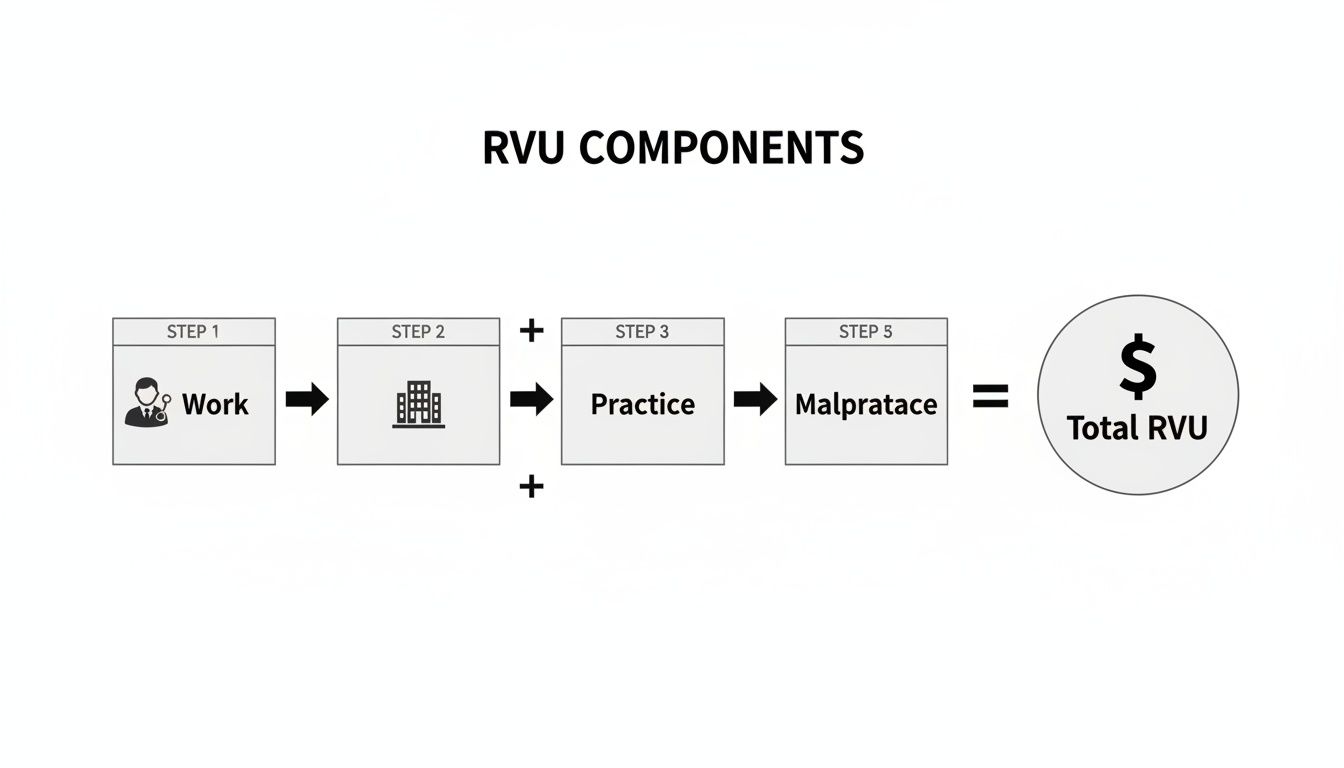
This process is designed to create payments that are fair, reflecting both the clinical effort involved and the real-world costs of running a practice in a specific part of the country.
Understanding the GPCI
The Geographic Practice Cost Index (GPCI) is a critical multiplier in the reimbursement formula. Its entire purpose is to adjust payments based on how much it costs to practice medicine in different regions. Let's be honest, it costs a lot more to run a clinic in Manhattan than in rural Nebraska, and the GPCI is how the payment system reflects that reality.
CMS actually uses three separate GPCI values, one for each RVU component:
- Work GPCI: Adjusts for the regional cost of physician labor.
- PE GPCI: Adjusts for the cost of things like rent, medical supplies, and staff salaries.
- MP GPCI: Adjusts for the cost of professional liability (malpractice) insurance premiums.
By applying these specific multipliers, the system generates a payment that's much more equitable and tied to local economic conditions.
The All-Important Conversion Factor
The final piece of the puzzle is the Conversion Factor (CF). Think of it as the master key that turns the total adjusted RVU value into a final dollar amount for Medicare payments. It's a single, national figure that the Centers for Medicare & Medicaid Services (CMS) updates every year.
The CF is also a major lever for controlling overall healthcare spending. Before 1992, physicians largely set their own rates, which led to massive inconsistencies. The CF brought much-needed standardization. This number isn't static; it has seen notable shifts over the years, declining from $34.8931 in 2021 to a projected $32.3465 in 2025, reflecting broader changes in healthcare policy and economics.
Putting It All Together: A 99213 Example
To make this tangible, let’s walk through a real-world example. We'll calculate the reimbursement for one of the most common services in primary care: CPT code 99213, an established patient office visit.
For this scenario, we'll use the national 2024 non-facility values and some sample GPCI values for Chicago, IL.
- Work RVU: 1.30
- Practice Expense (PE) RVU: 1.76
- Malpractice (MP) RVU: 0.08
Now, let's apply the hypothetical GPCI values for Chicago:
- Work GPCI: 1.018
- PE GPCI: 1.111
- MP GPCI: 0.547
Finally, we'll use the 2024 Medicare Conversion Factor of $32.74.
The table below breaks down the calculation step by step, showing how each component is geographically adjusted before being summed up.
Sample RVU Calculation for CPT Code 99213 (Established Patient Office Visit)
| Component | National Value (RVU) | GPCI (Chicago, IL) | Geographically Adjusted RVU |
|---|---|---|---|
| Work RVU (wRVU) | 1.30 | 1.018 | 1.3234 |
| Practice Expense (PE) RVU | 1.76 | 1.111 | 1.9554 |
| Malpractice (MP) RVU | 0.08 | 0.547 | 0.0438 |
| Total Geographically Adjusted RVU | 3.3226 |
With the total geographically adjusted RVU calculated, the final step is to apply the conversion factor.
3.3226 (Total RVUs) * $32.74 (CF) = $108.79
So, based on these values, the Medicare payment for a 99213 office visit in Chicago for 2024 would be approximately $108.79. This clear calculation shows exactly how each component directly influences the final payment you receive.
Beyond just crunching the numbers, it's vital to ensure that all claims are submitted correctly. Following robust medical billing compliance guidelines is paramount for preventing costly errors and maintaining the financial health of your practice.
Translating Your wRVUs into Your Salary
So, how does all this math actually turn into a paycheck? This is where the rubber meets the road.
While the practice cares about the total RVU reimbursement to keep the lights on, what you'll care most about is the Work RVU (wRVU). For most employed physicians, this is the magic number because your compensation is directly tied to how many wRVUs you generate. It's a clear, straightforward link between your clinical work and your income.
At the center of it all is the pay-per-wRVU rate. This is the dollar amount your employer agrees to pay you for every single wRVU you produce. This rate isn't set in stone; it's a critical part of your contract negotiation and can swing pretty wildly depending on your specialty, where you practice, and how in-demand your skills are.
The Basic Compensation Formula
At its core, the calculation is simple multiplication. Here's the formula you need to know:
Total Annual wRVUs Generated × Contracted $/wRVU Rate = Total Compensation
Let's run a quick scenario. Say you're an internist, and your contract offers a rate of $60 per wRVU. If you knock out 5,000 wRVUs in a year, your total pay comes out to $300,000.
Example Calculation:
- Total Annual wRVUs: 5,000
- Pay Rate: $60/wRVU
- Calculation: 5,000 wRVUs × $60/wRVU = $300,000
This direct connection is exactly why you need to be diligent about tracking your wRVUs. Every single service you provide, from a quick follow-up to a major procedure, adds to your bottom line.
How Everyday Work Adds Up
To bring this down to a daily level, think about that common CPT code 99213 for an established patient visit. In 2024, it's worth 1.30 wRVUs.
If your entire day was just seeing these types of patients, you'd need to see about 8 or 9 of them to generate around 11 wRVUs. Over a full work year, that consistent daily effort is what gets you to bigger targets like the 5,000 wRVUs in our example. Of course, your days will be more varied, but it shows how routine work steadily builds up.
Common Compensation Structures You Will Encounter
A straight pay-per-wRVU model is popular, but it's not the only game in town. Employers often use hybrid structures to offer a bit of a safety net while still encouraging productivity.
- Base Salary + Productivity Bonus: This is a classic. You get a guaranteed base salary, providing stability. Once your wRVU generation "covers" that base, any additional wRVUs you produce trigger a bonus payment. It gives you peace of mind with the upside of a bonus.
- Tiered Models: These are designed to really motivate high-performers. For instance, you might earn $55 per wRVU for your first 4,000 wRVUs, but the rate jumps to $65 per wRVU for anything you generate above that threshold. It’s a powerful incentive to push past your targets.
- Draw Against Production: With this model, you get a regular paycheck (the "draw"), which is basically an advance on your future earnings. Periodically (say, every quarter), the practice reconciles your actual wRVU earnings against what you were paid. If you earned more than your draw, you get a check for the difference. If you earned less, you might owe that money back.
Getting familiar with these different models is crucial when you're comparing job offers. To really dig into the numbers and see how different structures could play out for you, our physician salary calculator is a great tool for modeling these scenarios.
Navigating Modifiers and Other Real-World Complexities
The neat formulas for calculating RVUs are a great starting point, but clinical work is rarely that simple. A standard office visit can get complicated fast, and the RVU system has built-in ways to account for the messiness of real-world medicine. These usually come in the form of CPT modifiers and specific billing rules that can seriously alter your final wRVU count.
If you ignore these variables, you're almost certainly leaving earned wRVUs on the table. Knowing how to navigate them is key to making sure your compensation actually reflects the work you're doing.
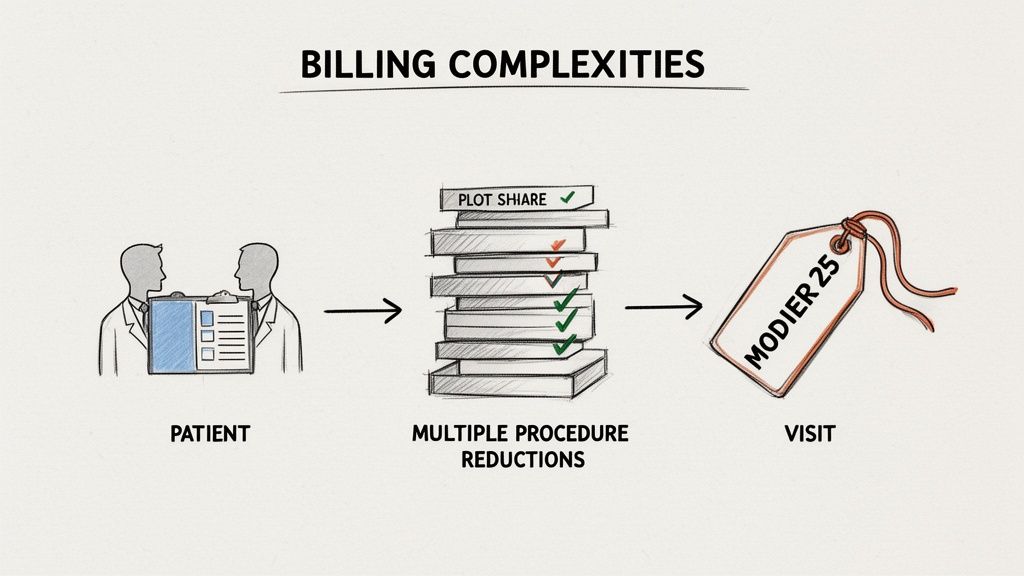
The Power of CPT Modifiers
CPT modifiers are two-digit codes you tack onto a primary CPT code. They signal that a service was altered in some way without changing its core definition. Think of them as a quick note to the payer explaining special circumstances—and some have a direct impact on your wRVUs.
One of the most common—and important—modifiers you'll run into is Modifier 25.
- Modifier 25: Significant, Separately Identifiable E/M Service
This modifier is your best friend when you perform a minor procedure and a separate evaluation and management (E/M) service on the same day. For example, a patient comes in for a scheduled follow-up for their hypertension (a 99213 visit) but also asks you to remove an unexpected mole during the same appointment.
By adding Modifier 25 to the 99213 code, you're telling the payer that the office visit was a distinct service from the mole removal. This allows you to get full wRVU credit for both the E/M service and the procedure. Without it, the E/M service would likely get bundled and denied.
Another key rule is the Multiple Procedure Reduction. When you perform several procedures in the same session, payers won't reimburse 100% for each one. The highest-valued procedure gets paid in full, but subsequent procedures are typically cut, often to 50% of their usual value. This reduction directly hits reimbursement, which can impact your compensation if your model is tied to collections.
Split Shared Billing in Team-Based Care
The way we deliver care is changing. Physicians, Nurse Practitioners (NPs), and Physician Assistants (PAs) are collaborating more closely than ever, which is where split/shared billing rules come into play. These CMS rules dictate how a service can be billed when it’s jointly managed by both a physician and a non-physician provider (NPP) in a facility setting.
For a visit to be billed under the physician, they must perform the "substantive portion" of the encounter. As of 2024, this means the physician personally handled the majority of the E/M visit (more than half the total time) or the medical decision-making.
When the criteria are met and billed under the physician, the service generates 100% of the associated wRVUs. If billed under the NPP, it typically generates only 85% of the wRVUs and reimbursement. Getting this right is absolutely essential for accurate RVU attribution in team-based models.
This system is always being refined. The responsibility for updating these values falls to groups like the Relative Value Scale Update Committee (RUC), which was formed back in 1991. The RUC plays a key role in calculating RVUs for new and revised codes by comparing the physician work required to existing services, ensuring things stay consistent across thousands of codes.
Generated RVUs vs. Actual Collections
Finally, it’s critical to understand the difference between productivity and profitability. You can generate a massive number of wRVUs, but if your practice has a poor collection rate, that productivity won't translate into revenue. A practice that struggles with claim denials, coding errors, or patient billing simply won't collect the full value of the services provided.
This is a huge deal because your compensation, even if based on wRVUs, is ultimately paid from practice revenue. If the practice's collection rate is only 80%, your high wRVU numbers might not be sustainable for the business. That can put downward pressure on your compensation rate over time.
When you're evaluating an employer, asking about their collection rate is just as important as discussing the pay-per-wRVU.
Common RVU Questions, Answered
Once you get the hang of the formulas, the real questions start popping up. How does this actually work day-to-day? Let's walk through some of the most common things that trip clinicians up when they're dealing with RVU-based compensation.
Where Do I Find the Official RVU Values?
The single source of truth here is the annual Medicare Physician Fee Schedule (MPFS). It's published by the Centers for Medicare & Medicaid Services (CMS), and you can find any CPT code value using the official MPFS Look-Up Tool on their site.
You’ll also see this data repackaged in easier-to-read formats from professional groups like the AMA or AAPC. Just make sure you're looking at the file for the current calendar year. These values change annually, and using last year's numbers is a common mistake.
How Do Private Insurance Companies Use RVUs?
Good question. Even though the RVU system was built for Medicare, it's become the default language for valuing medical services across the board. Nearly every private insurance company builds its payment schedule on top of Medicare's RVU values.
The key difference is the Conversion Factor (CF). A private payer negotiates its own unique CF with your hospital or practice. So, while the RVU value for a service is the same, Blue Cross might agree to pay 120% of the Medicare rate, leading to a higher final reimbursement. This negotiated CF is one of the most important details in any payer contract.
What's the RVU for CPT Code 99213?
This is probably the most-billed code in all of outpatient medicine. For 2024, the national values for an established patient office visit (CPT code 99213) are:
- Work RVU (wRVU): 1.30
- Practice Expense (PE) RVU): 1.76
- Malpractice (MP) RVU): 0.08
Your compensation is almost always tied directly to that 1.30 wRVU figure. The practice, however, gets reimbursed based on the total of all three components after geographic adjustments. This code represents a low-complexity visit, appropriate for addressing one or two stable chronic problems or an uncomplicated acute issue. Accurate documentation is key to ensuring a 99213 is justified and that the RVUs are captured correctly.
Do I Need to Care About PE and MP RVUs?
If your contract is pure wRVUs, then no, the PE and MP components won't directly affect your paycheck. But they are absolutely critical to the financial health of the practice you work for.
Think of it this way: your wRVUs determine the size of your slice of the pie. The Total RVUs (wRVU + PE + MP) determine the size of the entire pie itself. Your practice's revenue—which has to cover your salary, your MA's salary, the rent, and the light bill—is based on the Total RVU reimbursement.
While you're tracking wRVUs for your bonus, your employer is tracking Total RVUs to make sure the business stays afloat. A practice that doesn't generate enough Total RVU revenue can't afford to pay you.
Is My Pay-Per-wRVU Rate Negotiable?
Yes. One hundred percent. This is one of the most critical and negotiable numbers in your entire employment contract. Don't just accept the first number they give you.
Before you even think about negotiating, you need data. Look up the benchmark compensation stats for your specialty and region from a reputable source like the Medical Group Management Association (MGMA). Knowing the median and 75th percentile pay rates gives you the confidence and leverage to ask for what you're worth. Our own physician offer analyzer is designed to help you run these numbers. When you walk into a negotiation with hard data, it shows you've done your homework and are serious about getting a fair, evidence-based contract.
At WeekdayDoc, we're committed to helping you build a sustainable and rewarding career. Find burnout-friendly roles with transparent salary data and take control of your work-life balance at https://www.weekdaydoc.com.